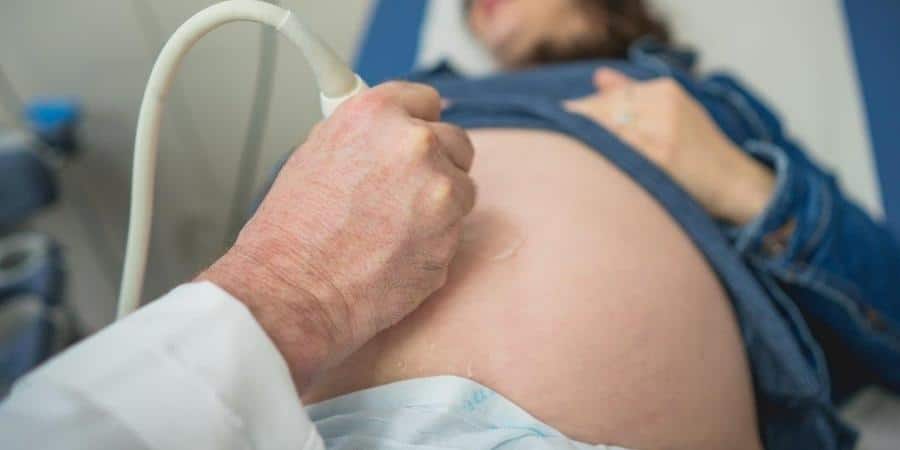
In the particular case of this woman, spina bifida was diagnosed when she was 20 weeks pregnant. After a detailed evaluation done with the aid of ultrasound and MRI, her doctors recommended that she undergo a new type of endoscopic surgery to repair the defect. The woman and her husband consented to this advanced procedure, and the Sheba staff began extensive preparations for the surgery. Over the course of several weeks, they consulted with doctors from the Texas Children’s Hospital in Houston, TX, including Dr. Michael Belfort, the physician who pioneered this surgical method.

A multidisciplinary team at Sheba helped to plan for the surgery, including the directors of the Gynecology and Maternity Division, Prof. Eyal Sivan and Prof. Shalev Mazaki, and leading members of the Fetal Medicine Unit, Prof. Yoav Yanon, Prof. Shlomo Lipitz, Prof. Boaz Weiss, Dr. Hagai Avnet, and Mrs. Iris Horowitz. In addition, Dr. Jacob Zauberman, pediatric neurosurgeon, Dr. Gil Har-Zahav, pediatric surgeon, Dr. Dina Orkin and Dr. Arkady Shraga, anesthesiologists, Dr. Eldad Katorza, imaging expert, and surgical nurses Ms. Aviva Asher and Ms. Dekla Pasternak collaborated to ensure that the hospital facilities were fully ready for the cutting-edge procedure.
When the woman reached her 25th week of pregnancy, the operation was performed. Three physicians from the Texas Children’s Hospital travelled to Sheba to assist. During the surgery, two trocars were used to make an abdominal opening to access the uterus and conduct amniocentesis, CO2 gas extraction, and endoscopic repair of the spinal defect. The operation proceeded normally, and after discharge, the woman was monitored weekly in the Fetal Medicine Unit.
Follow-up imaging tests showed significant improvement in cerebral herniation. At 30 weeks of pregnancy, the woman was hospitalized for low amniotic fluid, and at 31 weeks + 4 days, she gave birth to a healthy baby girl (1677 grams) via C-section. The infant was hospitalized and monitored after birth, and no complications were detected. Now, the child is nine months old, with normal leg mobility and no need for a brain shunt.