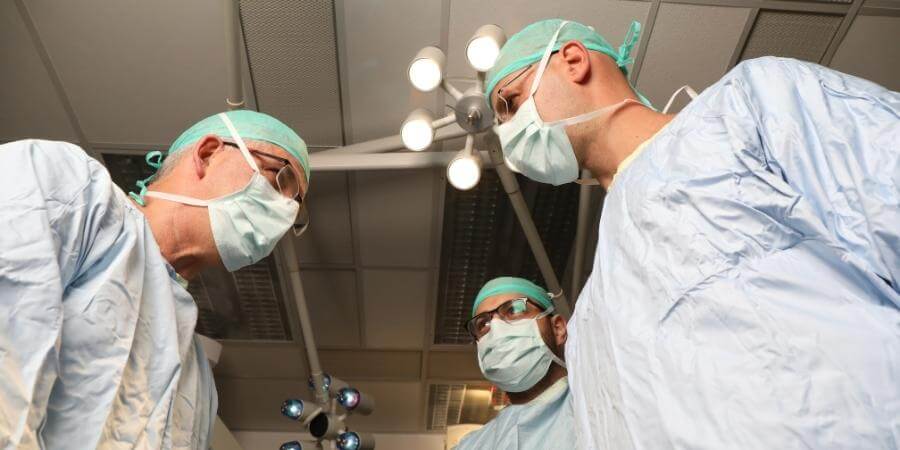
For the first time in Israel, doctors at Sheba Medical Center performed a new, cutting-edge procedure on a patient with a malfunctioning mitral valve: a transcatheter mitral valve replacement (TMVR).
During a TMVR, doctors replace defective mitral valves with an artificial substitute through catheterization, using a new technique called LAMPOON, which prevents the obstruction of blood flow in the left ventricular outflow tract (LVOT): a common fatal complication of TMVR. The LAMPOON procedure involves inserting two catheters through blood vessels in the patient’s groin and up to the heart, then using an electrified wire woven through the catheter to split open the heart valve leaflet and replace the valve.
For elderly or frail patients, TMVR offers a less-invasive alternative to open-heart surgery. It was recently performed at Sheba on a 74-year-old patient who suffers from a cardiovascular connective tissue disease and underwent open-heart surgery 14 years ago.
The non-invasive procedure, which was completed successfully with no serious complications, was conducted by Sheba’s Prof. Victor Guetta, Director of the Invasive and Interventional Cardiology Unit, along with Prof. Israel Barbash, Director of Catheterization Services. Having extensive experience with the LAMPOON technique, Dr. Robert Lederman, Chief of the US National Heart, Lung, and Blood Institute, and Head of the Cardiovascular Intervention Laboratory, along with Dr. Adam Grinbaum, Co-Director of the Structural Heart and Valve Center at Emory University, monitored the procedure through bidirectional audiovisual telecommunication and guided the catheterization team in real-time.
According to Prof. Guetta, “The patient’s mitral valve deteriorated over time. Theoretically, he could have undergone another surgery, but since the patient already had an invasive open-heart surgery previously, there would be a greater chance of fatal complications.”
Prof. Israel Barbash added, for his part: “This procedure is a leap forward in our ability to offer treatment options to people who, until now, have been unable to receive proper care for this kind of illness.”