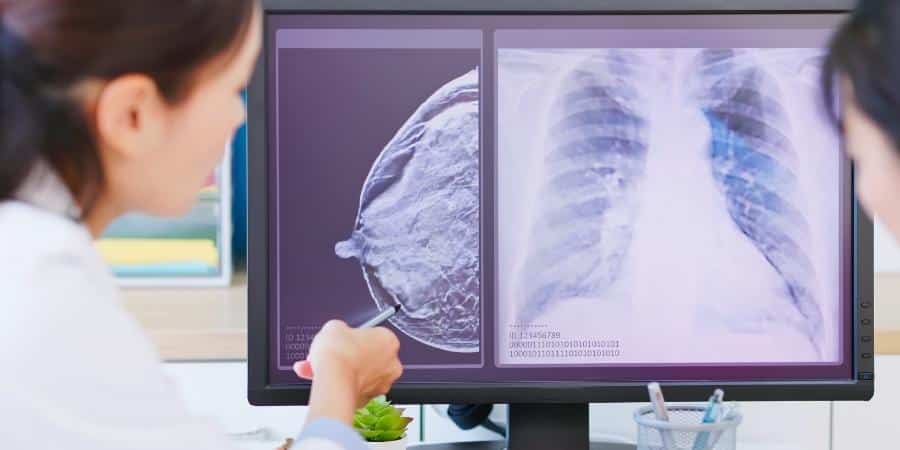
The American Journal of Roentgenology recently published a study co-authored by Dr. Miri Sklair-Levy, director of Sheba’s Breast Imaging Unit. The results showed that contrast-enhanced mammography (CESM) and ultrasound detected approximately twice the amount of cancers that breast MRIs typically identify, as well as several more cancers than generally detected by traditional mammography. The study was conducted at Sheba Medical Center from 2012 to 2017, and over 600 Israeli women participated. These patients all had dense breast tissues and were considered to be at “intermediate risk” of developing breast cancer.
CESM is recommended in particular for women who have dense breasts, such as young women. Conventional mammography displays dense breast tissue as solid white, while non-dense tissue shows up as dark and transparent. This white imagery makes it difficult to distinguish tumors from healthy tissue. When mammography is inconclusive, women are generally advised to undergo additional testing. However, the use of contrast mammography eliminates the need for many of these additional diagnostic procedures because it shows a more comprehensive view.
“We know that mammography misses up to 30% of cancers, specifically in women with dense breasts, implants, or who had previous surgery. When mammography and ultrasound are used together, the rate of missed cancers drops,” said Dr. Sklair-Levy. “When contrast imaging is used, it enables a view of the metabolism or activity of the tissues. Cancers have a higher blood supply than other cells, so when we see an increase in blood supply, it raises the suspicion of cancer.”
Statistically, CESM testing identifies 13-15 cancers in every 1,000 women. This is in significant contrast to conventional mammography, which identifies about 4 cancers in every 1,000 women who undergo screening. When women undergo screening with both conventional mammography and ultrasound, that amount goes up to 8 cases. MRIs diagnose 15 cancers per 1,000 women. However, many women dislike the experience of MRIs, which can be claustrophobic and provoke anxiety.
“Women prefer CESM,” said Dr. Sklair-Levy. “It’s faster and unlike an MRI, it doesn’t require the patient to be in a closed machine … Today, no one is diagnosing cancer in other organs without contrast media.”
The Sheba study, part of which was also published recently in the Journal of Clinical Radiology, evaluated whether the use of routine ultrasounds along with CESM enhanced the identification of breast cancer. The results demonstrated that when suspicious lesions were detected by CESM, it was considered appropriate to follow up with an ultrasound and a biopsy. When a lesion that was found with CESM appeared benign, the routine recommendation of ultrasound was considered questionable, because it could lead to unnecessary biopsies.
The Meirav Breast Center treats more breast cancer patients than any other cancer center in Israel. The high-risk clinic performs a yearly breast MRI for all patients who have tested positive for the BRCA1 and BRCA2 gene mutations. Dr. Sklair-Levy hopes to soon be able to provide the CESM test for every patient considered to be at high-risk. “The clearer the image, the lower the need for unnecessary biopsies,” she added.
CESM is not suitable for any patient with impaired renal function or with an allergy to iodine. In addition, the use of contrast gadolinium has not been proven safe to a fetus, and therefore pregnant women are not candidates for CESM. However, researchers at the Meirav Breast Center are currently exploring better ways to test for cancer in pregnant women.