3D printing technology enables the computerized creation of 3D models directly from engineering plans. One of the most beneficial applications of this innovative technology is in the field of medicine, particularly surgery. A 3D printer can be used to create customized prosthetic limbs, organ facsimiles and specialized surgical tools. It offers unparalleled opportunities for personalized precision medicine, helping to prepare doctors for complex, invasive procedures.
With a keen eye for embracing the latest technological innovations for healthcare, Prof. Yitshak Kreiss, Director General of Sheba Medical Center, commissioned Dr. Dina Orkin, the director of Sheba’s 30 operating rooms, to head the new 3D lab. Prof. Kreiss’s goal is to change the face of conventional medicine.
To date, the 3D team at Sheba has already printed a variety of personalized prosthetic implants for hip and knee replacements.
The outcomes have been impressive, leading Dr. Orkin to believe that the future of orthopedic surgery lies in 3D-printed components, as opposed to mass-produced elements that cannot provide a perfect fit for each patient.
Omer, a five-year-old boy suffering from Ewing sarcoma, is one amazing example of just how Sheba implemented 3D printing as a true game-changer for his quality of life. Ewing sarcoma forms in bone and soft tissues, and Omer needed to have his leg amputated to remove the malignant bone tumor.
“In this case, we printed a mold (think cake pan) that corresponds exactly to the affected bone, filled it with surgical cement and voila – a precise ‘custom made’ femur, perfectly suited to the patient,” explained Orkin. “After rehab, this child will be able to stand on his feet, walk, and even run. He’ll have the gift of a childhood.”

The 3D printing lab is also used for oral and maxillofacial reconstruction, which involves repairing defects in the face and jaw. When a 50-year-old man suffering from a severe toothache was diagnosed with a tumor in his lower jaw, part of the mandible had to be surgically removed. The maxillofacial surgeon used 3D-printed measuring guides to cut bone grafts from the patient’s leg, enabling higher precision for the size and shape, as well as determining the optimal angle for the incision.
Dr. Orkin shared how this process eliminated the usual trial and error, with no leftover bone. “The pieces fit together like Lego,” she said.
Regarding results and recovery time, the patient also experienced a relatively fast recovery, without the difficulty chewing and impaired speech normally associated with similar operations.
Another boon of 3D printing technology is that it allows patients to view computer-simulations of different possibilities for facial reconstructions, and then choose the features they want. The medical team can print components according to the patient’s specifications.
Dr. Orkin had dreamed of being a doctor since she was a young child. “For as long as I can remember, I wanted more than anything to work in the operating room,” she shared. “In high school, I was able to get a job cleaning the operating rooms in a university hospital close to our home. I always felt my heart beating in anticipation whenever I crossed the red line that separated the waiting room and the doors to the OR — and I was only there to wash the floor.”
Eventually, Orkin fulfilled her dream, first specializing in anesthesiology in the ICU and serving as Director of Pediatric Anesthesiology at Shaare Zedek Medical Center in Jerusalem. But she felt the need to move on and transferred to Sheba, where her creativity and inventive thinking were recognized. At Sheba, she was able to implement her vision of the OR as a multidisciplinary system under one central managing hub, which functions around the needs of the patient front and center.
“Of course, I don’t do it all alone. I’m surrounded by people who believe in me and what I do, and who want to be part of this. At the end of the day, we all see our work not as a job, but as a mission, and we all work together,” she said.
The technology for effective 3D printing is already available, but Dr. Orkin stresses that it will take time to mainstream this method. Personalized printing is expensive, and the need for quality control is even greater. While internal organs cannot yet be printed out of tissue cells, that too is in development.
“My hope for the future is for a company like Johnson & Johnson [the manufacturers of titanium
hip replacements] to start producing their own regulated, 3D printed prosthetic implants,” she said.
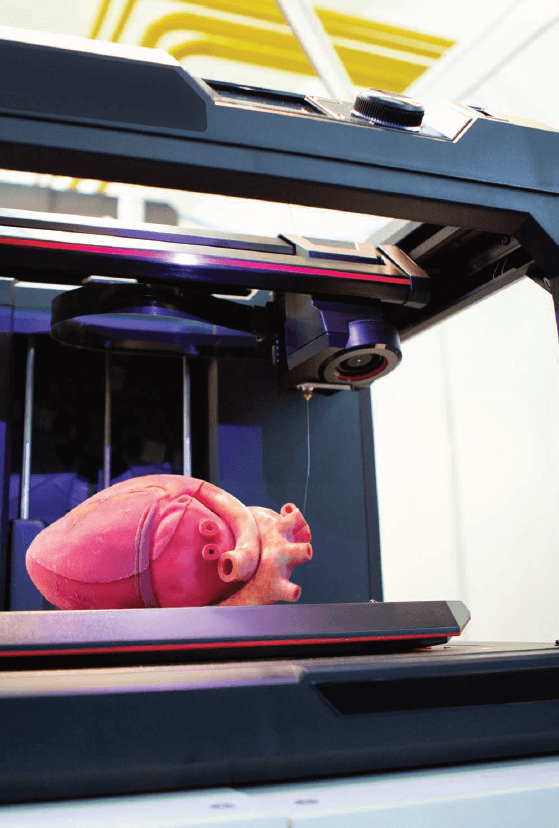
Another surgical application of 3D printing is the ability to order customized organ facsimiles.

By producing a flexible polymer replica of a patient’s heart, a surgical team can determine the precise location and angle for performing complex procedures such as a heart transplant, thereby making the procedure less challenging.At Sheba, this technique was used to help a 14-year-old girl with end-stage heart failure to finally receive the life-saving heart transplant she was waiting for.
“After spending two years in and out of the hospital, she is finally back home and leading a normal life,” said Orkin.
3D images don’t always require printing. Physicians can also view the images in a virtual reality (VR) software. They wear specialized goggles that allow manipulation of the images on screen. Augmented reality is integrated into these programs, providing computerized images with different levels of transparency, so physicians can “see” layers of the inner anatomy.
The potential of 3D printed bone and organ facsimiles is wondrous and overwhelming, helping doctors to prepare for surgeries, reducing time in the operating room and enhancing patient recovery and quality of life.