Neurosurgery – Brain and Spinal Surgery
Neurosurgery – Brain and Spinal Surgery
Neurosurgery at Sheba Medical Center is provided within the Division of Surgery and offers premier care for patients in all neurosurgical subspecialties. We perform cerebrovascular surgery, radiosurgery, stereotactic and functional surgery, spinal surgery, and pediatric neurosurgery, as well as manage head and spinal cord trauma.
Our Neurosurgery Unit contains many state-of-the-art clinics, all staffed by a select team of brain and spine specialists and equipped with the latest technologies. We are dedicated to advancing neurosurgery through clinical research and the development of new, advanced techniques.
We offer neurosurgery for the following conditions:
Hydrocephalus
Hydrocephalus refers to the buildup of fluid in the ventricles within the brain; this excess fluid puts pressure on the brain. Normally, cerebrospinal fluid flows through the ventricles, moistening the brain and spinal column. However, too much of this fluid can damage the brain and impair function. Hydrocephalus occurs most commonly in infants and adults over 60.
The surgical insertion of a shunt, a drainage system, is the most common treatment for hydrocephalus. The shunt is a long, flexible tube with a one-way valve that prevents fluid from the brain from flowing in the wrong direction. Generally, one end of the tube is placed in one of the ventricles of the brain and then channeled under the skin to another part of the body, such as the abdomen, where the fluid can be easily absorbed. The shunt system usually remains in place for the rest of the person’s life, and regular monitoring is necessary. Possible complications include mechanical malfunctions, infections, and blockage that interferes with the proper drainage of cerebrospinal fluid.
Pituitary Tumors (Adenomas)
A pituitary tumor is an abnormal growth in the pituitary gland, which can cause an overproduction or underproduction of important hormones. The majority of pituitary tumors are benign growths, called adenomas, which stay local and don’t spread to other parts of the body.
Surgical removal of a pituitary tumor is typically necessary if it is causing the overproduction of specific hormones or pressing on the optic nerves. Sheba surgeons will perform endoscopic transnasal transsphenoidal surgery to remove the tumor through the nose and sinuses, thereby avoiding an external incision. When the nostrils are too small or distorted, this surgery may be done through an incision under the upper lip. Our neurosurgeon will use specialized microsurgery devices and a microscope to magnify the field of surgery, identify, and precisely remove the adenoma safely from nearby healthy tissue.
Transsphenoidal surgery does not affect any other part of the brain. However, it can be very difficult to remove a large tumor using this approach, especially if it has penetrated brain tissue or any surrounding nerves.
Herniated Disk
A herniated disk occurs when there is a problem with one of the disks (rubbery pads) that rests between the individual vertebrae of the spine. Although aging and disk degeneration are the typical causes of disk herniation, most of the time the precise culprit of disk herniation cannot be identified.
Each spinal disk consists of a tough, rubbery exterior that surrounds a central jellylike nucleus. When a herniated disk (also called a slipped disk or ruptured disk), occurs, it means that some of the inner nucleus has pushed out through a tear in the disk exterior. This can happen in any region of the spine, and sometimes it irritates a nerve – causing numbness, weakness, or pain in a leg or arm. When that happens, surgery may be required to relieve the problem.
Depending on the patient’s specific condition, surgery for a herniated disk can be:
- Laminectomy – our neurosurgeon will remove the lamina (the back part of a vertebra that covers the spinal canal) to create space. This relieves pressure from the spinal cord or nerves.
- Discectomy – in this procedure, the damaged part of a herniated disk is removed in order to relieve pressure from a spinal nerve and treat pain that radiates down the legs or arms; it is not generally done to relieve neck or back pain.
Spinal Stenosis
Spinal stenosis refers to a narrowing of the spaces in the spine, and it occurs most commonly in the lower back and neck. As a result, pressure may be placed on the nerves that go through the spine. Spinal stenosis is usually caused by normal wear and tear related to osteoarthritis. Sometimes it leads to pain, tingling, muscle weakness, and numbness, while other times it is asymptomatic. In severe cases, surgery may be recommended to restore the collapsing disk space in the spinal canal, making more room for the spinal cord or nerve roots.
To decompress the spinal cord and/or spinal nerve and enable the nerves to heal, Sheba neurosurgeons may perform a discectomy and fusion. This surgical procedure involves removing the degenerated disk and fusing the adjacent vertebrae. Alternatively, minimally invasive options done with a laparoscopic, abdominal approach may be suitable.
Craniotomy (Head surgery)
A craniotomy is the surgical removal of part of the skull bone to provide access to the brain. Using specialized tools, a bone flap is made and temporarily removed – to be replaced after the brain surgery is finished. Sheba neurosurgeons perform computer-guided craniotomy using imaging to help reach the exact location that needs treatment in the brain.
Craniotomies may be performed to remove large or complicated brain tumors, as well as for clipping an aneurysm to preventing a rupture. This procedure may also be necessary in cases of intracerebral hemorrhage in order to drain the bleeding.
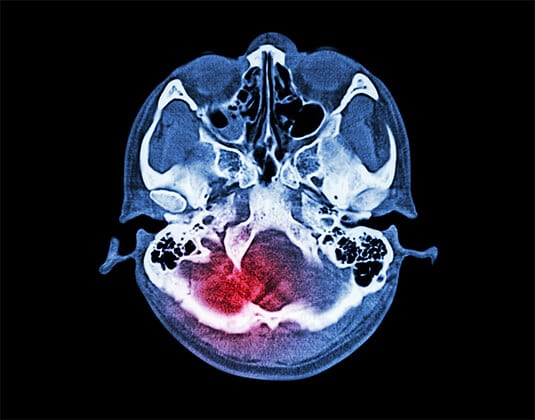
Why Choose Sheba for Neurosurgery in Israel?
The Department of Neurosurgery at Sheba is one of the largest neurological centers in the world. We perform approximately 1,200 surgical procedures every year. Our staff comprises world-renowned experts who trained at leading medical facilities, and they are skilled in applying the latest technologies and frontline surgical techniques. Whenever possible, we strive to perform treatment with minimally invasive procedures to promote easier, faster recuperation. In addition to our premier skill, we also practice medicine with a compassionate, personal touch – custom-designing treatment programs to meet the needs of each individual patient, before, during, and after surgery.
Sheba is committed to holistic healthcare that considers your quality of life as you undergo neurosurgery for your medical condition. Supportive services, including social workers, nutritionists, and rehabilitation professionals, conveniently offer therapies on our all-inclusive campus. To help facilitate a smooth experience, we assign every patient a personal medical coordinator from the International Medical Tourism Division. Your coordinator will provide assistance with every step of your arrangements, treatment, and follow-up at Sheba.

Our Staff



Related Doctors

Academic experience: 2015-present, lecturer at the Tel-Aviv

Dr. David Hazzan manages the minimally invasive and robotic

Dr. Barak Rosenzweig is a senior physician in the Department

Prof. Eytan Mor is an expert in kidney, liver and pancreas t
Request a consultation
Sheba Medical Center provides innovative, personalized medical care to patients from around the world. We are the largest, most comprehensive hospital in the Middle East and dedicated to providing advanced and compassionate medicine for everyone.
We welcome all cases, including the rarest and the most challenging. Our medical teams collaborate to provide the best possible health outcomes. From your initial inquiry through the long-term follow-up care, we are here for you.
Request a consultation and a Sheba Case Manager will contact you shortly:
