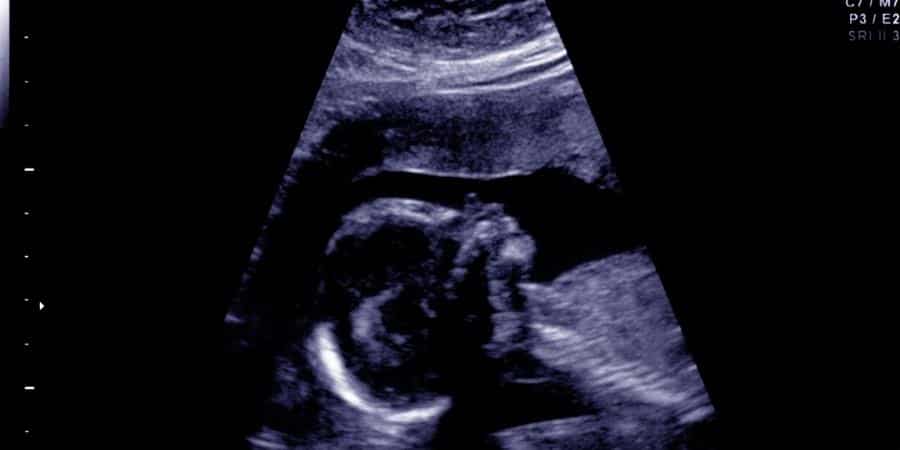
The mother was already a known hemophiliac and was treated at the National Hemophilia Institute at Sheba Medical Center. The fetus was diagnosed with hemophilia during a chorionic villus sampling (CVS) examination. Later, he was also diagnosed with anemia during a follow-up, making for a dangerous combination.
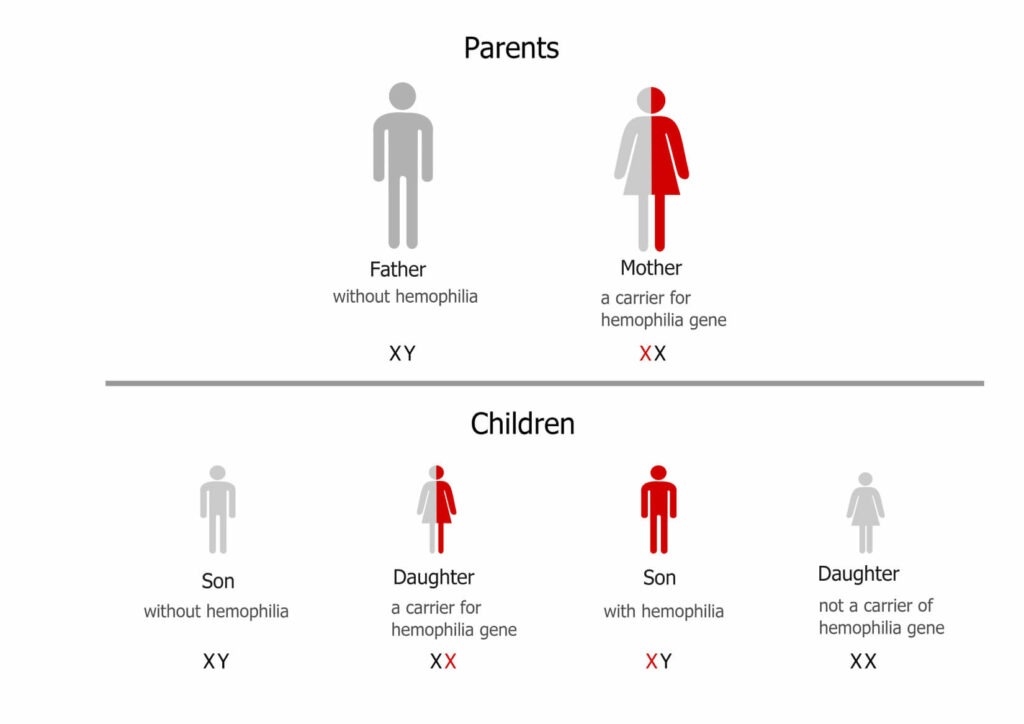
Hemophilia is a blood clotting disorder caused by a missing protein in the clotting pathway. Patients with hemophilia may suffer from spontaneous bleeding of the muscles and joints and are especially prone to uncontrolled bleeding during or after surgical procedures.
Anemia in the fetus developed following the formation of antibodies in the mother that attacks the fetal blood cells. These antibodies pass from mother to fetus and cause the destruction of the blood cells, thus leading to anemia in the fetus. This condition can cause heart failure and most often results in death.
In order to treat these dual problems, the fetus needed a blood transfusion. However, hemophilia presented a particularly high risk for life-threatening bleeding.
The procedure was performed several times, beginning in the 24th week of pregnancy. A certain blood clotting factor, Factor IX, was injected into the fetus’ umbilical cord as well as introduced via blood transfusion. This strengthened the clotting mechanisms and allowed the fetus to avoid severe and life-threatening bleeding.
The complex and delicate procedure was carried out by the specialists in the Unit for Fetal Medicine – Prof. Shlomo Lipitz, Prof. Boaz Weiss, and Prof. Yoav Yinon, in the presence of a hematologist, Dr. Shadan Lalezari of the National Hemophilia Institute headed by Prof. Gili Kenneth.
Prof. Weiss summarized the case, “We perform blood transfusions to fetuses in about 15 cases each year. Hemophilia in a fetus is a situation we are familiar with, but this combination of symptoms and the difficulty of performing the invasive procedure is rare.”
Prof. Yoav Yanon: “The two phenomena are very rare and there is no similar situation and procedure documented in the medical literature. The infusion carries a risk that the fetus might bleed to death. Therefore, in coordination with Prof. Kenneth and Dr. Lalezari, we decided to inject the missing coagulation factor to reduce the risk of bleeding during the procedure.
The fetus underwent three intrauterine transfusions during weeks 24, 27, and 30 and was safely delivered in week 34. This positive outcome is thanks to the unique process, the original thinking, and the mobilization of various teams in support of the patient.”
Prof. Gili Kenneth noted, “This is the first case in the world reported where blood transfusions along with a thrombosis factor were provided through the umbilical cord to a hemophiliac patient. Furthermore, this groundbreaking procedure makes our patient the youngest ever to have received a coagulation factor “.
The baby was born in the 34th week of pregnancy by Caesarean section. After the birth, the baby was found to have a low Factor IX level and was treated with another transfusion of coagulation concentrate in order to safely undergo circumcision.
The baby continues to be treated at the National Hemophilia Institute at Sheba, which treats about 700 patients with hemophilia gene therapy in Israel and is considered a leading international institute for treatment quality and advancement of research in the field.