Researchers in a laboratory at Tel Aviv University (TAU) demonstrated that the CRISPR -Cas9 system is very effective at treating metastatic cancer. CRISPR-Cas9 is a high precision gene-editing technique that can change the DNA of animals, plants and microorganisms. Theoretically, a precise part of any chosen genome can be spliced, allowing the use of the cell’s natural systems to manipulate gene coding and rewrite the code of life.
In a recent research study in Israel, scientists developed a novel lipid nanoparticle-based delivery system that targets cancer cells and uses genetic manipulation to destroy them. The breakthrough system is called CRISPR-LNPs, and it carries messenger RNA that encodes for the CRISPR enzyme Cas9, which acts as molecular scissors to snip the cancer cells’ DNA.
“This is the first study in the world to prove that the CRISPR genome editing system can be used to treat cancer effectively in a living animal,” said Prof. Dan Peer, VP for R&D and Head of the Laboratory of Precision Nanomedicine at the Shmunis School of Biomedicine and Cancer Research at TAU. “It must be emphasized that this is not chemotherapy. There are no side effects, and a cancer cell treated in this way will never become active again. The molecular scissors of Cas9 cut the cancer cell’s DNA, thereby neutralizing it and permanently preventing replication.”
The groundbreaking research was conducted by Dr. Daniel Rosenblum, Ph.D., together with Ph.D. student Anna Gutkin and colleagues, in collaboration with Dr. Zvi R. Cohen, Director of Neurosurgical Oncology and Vice-Chair of the Department of Neurosurgery at Sheba Medical Center; Dr. Dinorah Friedmann-Morvinski from TAU; Dr. Mark A. Behlke, Chief Scientific Officer at IDT Inc.; and Prof. Judy Lieberman of Boston Children’s Hospital and Harvard Medical School. It was carried out in Prof. Peer’s Laboratory of Precision Nanomedicine.
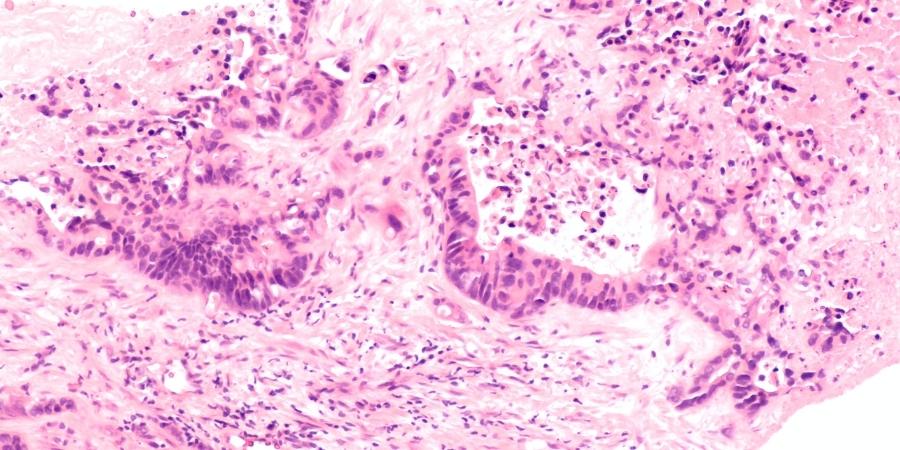
Prof. Peer and his team chose two of the deadliest cancers to examine for the potential of using the CRISPR-LNPs technology as a cancer treatment: metastatic ovarian cancer and glioblastoma. Glioblastoma, the most aggressive type of brain cancer, has an average life expectancy of only 15 months after diagnosis; the 5-year survival rate is only 3%. The research demonstrated that one solitary treatment with CRISPR-LNPs doubled the average life expectancy of mice with glioblastoma tumors, and their overall survival rate was boosted by about 30%.
Ovarian cancer has the highest fatality rate of all cancers of the female reproductive system and it is a major cause of death among women worldwide. Diagnosis is generally made at an advanced stage, when metastases have already spread throughout the body. Although recent scientific studies have led to notable progress in treating ovarian cancer, only a third of patients survive. Treatment with CRISPR-LNPs in mice with metastatic ovarian cancer increased their survival rate by 80%.
Prof. Peer explained that the CRISPR genome editing technology is capable of identifying and altering any genetic segment. This capability has revolutionized the ability to disrupt, repair or even replace genes – with a personalized approach. He adds, “Despite its extensive use in research, clinical implementation [of the CRISPR technology] is still in its infancy because an effective delivery system is needed to safely and accurately deliver the CRISPR to its target cells. The delivery system we developed targets the DNA responsible for the cancer cells’ survival. This is an innovative treatment for aggressive cancers that have no effective treatments today.”
The scientific researchers point out that this demonstration of how CRISPR -based genome editing can treat two aggressive cancers opens multiple possibilities for treating other types of cancer, in addition to rare genetic diseases and chronic viral diseases such as AIDS.
“It will probably take some time before the new treatment can be used in humans, but we are optimistic,” said Prof. Peer. “The whole scene of molecular drugs that utilize messenger RNA (genetic messengers) is thriving—in fact, most COVID-19 vaccines currently under development are based on this principle. When we first spoke of treatments with mRNA twelve years ago, people thought it was science fiction. I believe that in the near future, we will see many personalized treatments based on genetic messengers—for both cancer and genetic diseases.”
The results of the study, which was funded by the Israel Cancer Research Fund, were published in the November 2020 issue of Science Advances.